What is it erythema multiform?
Erythema multiforme is a hypersensitivity reaction usually triggered by infections, most commonly herpes simplex virus (HSV). It comes with a skin eruption characterized by a typical objective injury. There may be mucous membrane compromise. Is acute and self-limited, which usually resolves without complications.
Erythema multiforme is divided into major and minor forms and is now considered distinct from Stevens-Johnson. syndrome (SJS) and toxic epidermal necrolysis (TEN).
Who gets erythema multiforme?
Erythema multiforme most commonly affects young adults (20–40 years of age), however all age groups and races can be affected. There is a male predominance.
There's a genetic tendency to erythema multiforme. Certain types of tissue are found more often in people with herpes-associated erythema multiforme (HLA-DQw3) and recurrent erythema multiforme (HLA-B15, -B35, -A33, -DR53, -DQB1*0301).
What triggers erythema multiforme?
Infections
Infections are probably associated with at least 90% of erythema multiforme cases.
The most common trigger for developing erythema multiforme is the herpes simplex virus (HSV) infection, usually herpes labialis (cold sores on the lip) and less frequently genital herpes. HSV type 1 is more commonly associated than type 2. Herpes infection usually precedes skin rash by 3–14 days.
Mycoplasma pneumonia (a lung infection caused by bacteria Mycoplasma pneumoniae) is the next most common trigger.
Many different virus infections have been reported to trigger erythema multiforme, including:
- Parapoxvirus (orf and milkers nodules)
- Herpes varicella-zoster (chicken pox, shingles)
- Adenoviruses
- Hepatitis virus
-
Human immunodeficiency virus (HIV)
- Cytomegalovirus
- viral vaccines
Dermatophyte fungal infections (ringworm) have also been reported in association with erythema multiforme.
Drugs
Medications are probably a rare cause (<10%) de eritema multiforme. Si este diagnóstico se está considerando seriamente, entonces el medicamento alternativo rashes should be excluded, such as SJS/TEN, generalized fixed Drug Rash, polymorphic exanthematous drug eruption and urticaria.
Many drugs have been reported to trigger erythema multiforme, including barbiturates, non-steroidal anti-steroids.inflammatory drugs, penicillins, sulfonamides, nitrofurantoin, phenothiazines, and anticonvulsants.
Clinical features of erythema multiforme.
general symptoms
There is usually no prodromal symptoms in erythema multiforme minor. However, erythema multiforme major may be preceded by mild symptoms such as fever or chills, weakness, or joint pain.
Skin lesions
Typically, in erythema multiforme, a few to hundreds of skin lesions erupt in a 24-hour period. Lesions are first seen on the backs of the hands and/or tops of the feet and then spread down the extremities toward the trunk. The upper limbs are more commonly affected than the lower limbs. The palms and soles may be involved. The face, neck, and trunk are common sites. Skin lesions are often grouped on elbows and knees. There may be an associated mild itching or burning sensation.
The initial lesions are acutely demarcated, round, red/pink and flat (macules), which become raised (papules/ /palpable) and gradually expand to form plates (raised flat patches) up to several centimeters in diameter. The center of the papule/ /license plate darkens in color and develops superficial (epidermal) changes such as blisters or crust. The lesions generally evolve over 72 hours.
The typical target lesion (also called iris injury) of erythema multiforme has a sharp margin, a regular round shape, and three concentric color zones:
- The center is dark or dark red with a blister or Cortex
- The next ring is a paler pink and is raised due to edema (fluid swelling)
- The outermost ring is bright red.
Atypical target lesions show only two zones and/or an indistinct border.
The rash is polymorphous (many forms), hence the "multiform" in the name. Lesions may be in various stages of development with typical and atypical targets present at the same time. A full skin exam may be required to find typical targets, as these may be few in number.
The lesions show Kobner (isomorphic) phenomenon, which means that they can develop in previous sites (but not concurrent or later) skin trauma.
There is no associated swelling of the face, hands, or feet, despite being common sites of eruption distribution. However, the lips are often swollen, especially in erythema multiforme major.
Erythema multiforme
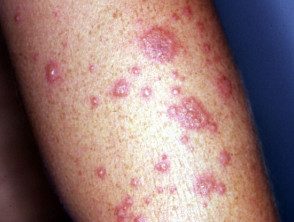
Erythema multiforme
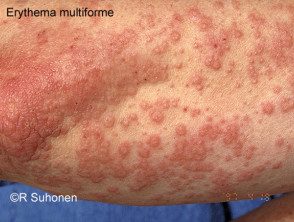
Target injuries
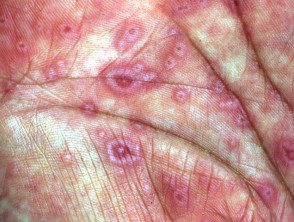
Target injuries
See more images of erythema multiforme.
Mucous membrane intervention
Mucous membrane Lesions, if present, usually develop a few days after the rash begins.
In erythema multiforme minor, mucous membrane involvement is absent or mild. Mucosal changes, if present, initially consist of redness of the lips and inside the cheek. Blisters sometimes develop and quickly rupture to form erosions and ulcers.
In erythema multiforme major, one or more mucous membranes are usually affected, most often the oral mucous membrane:
- Most commonly lips, inside of cheeks, tongue
- Less commonly floor of the mouth, palate, gums.
Other affected mucosal sites may include:
- Eye
- anus and genitals
- trachea / bronchi
- Gastrointestinal tract.
Mucosal lesions consist of swelling and redness with blister formation. The blisters quickly rupture to leave large, shallow, irregularly shaped, painful ulcers that are covered by a whitish pseudomembrane. Typically the lips are swollen with hemorrhagic scabs The patient may have difficulty speaking or swallowing due to pain.
With mycoplasma pneumonia, the mucous membranes may be the only sites affected (mucositis) This can be serious and require hospitalization due to difficulty eating and drinking. Whether this is a limited form of erythema multiforme has not been determined. Also known as Fuchs syndrome, mucosal erythema multiforme can occasionally be due to recurrent herpes simplex.
Erythema multiforme: mucosal involvement
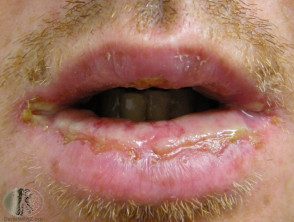
Erythema multiforme of the lips.
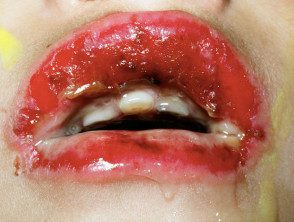
Erythema multiforme of the lips.
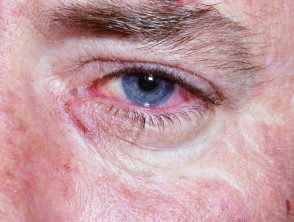
Erythema multiforme of the eye
Recurrent erythema multiforme
Erythema multiforme can be recurrent, with multiple episodes per year for many years. This is thought to almost always be due to HSV-1 infection.
How is the diagnosis of erythema multiforme made?
Erythema multiforme is a clinical diagnosis, although the skin biopsy may be required to exclude other conditions. the histology of erythema multiforme is characteristic but not diagnostic. It varies with the age of the lesion, its appearance, and which part is biopsied.
Other tests may be done to detect infections commonly seen in association with erythema multiforme, such as mycoplasma.
For more details, see Erythema Multiforme: Histology and Mechanisms.
Treatment of erythema multiforme
For most cases, no treatment is required, as the rash goes away on its own for several weeks without complications.
Treatment directed at any possible cause may be required, such as oral acyclovir (not current) for HSV or antibiotics (eg, erythromycin) for Mycoplasma pneumoniae. If the cause of a drug is suspected, then the possible offending drug should be stopped.
Supportive/symptomatic treatment may be necessary.
- Itching: Oral antihistamines and/or topical corticosteroids may help.
- Oral pain – mouthwashes containing local anesthetic and antiseptic reduce pain and secondary infection.
- Ocular involvement should be evaluated and treated by a ophthalmologist.
- Erythema multiforme major may require hospital admission for supportive care, particularly if severe oral involvement restricts alcohol consumption.
The role of oral corticosteroids remains controversial, as no controlled studies have shown any benefit. However, for severe disease, 0.5–1 mg/kg/day of prednisone or prednisolone is often used early in the disease process.
Recurrent erythema multiforme is usually initially treated with continuous oral acyclovir for 6 months at a dose of 10 mg/kg/day in divided doses (eg, 400 mg twice daily), even if HSV has not been a obvious trigger of the patient's erythema multiforme. . This has been shown to be effective in placebo-reviewed double-blind studies. However, erythema multiforme may recur when acyclovir is discontinued. Other antiviral medications such as valacyclovir (500–1000 mg/day) and famciclovir (250 mg twice daily) should be tried if acyclovir has not helped; These drugs are not available in New Zealand.
Other treatments (used continuously) that have been reported to help suppress recurrent erythema multiforme include:
-
Dapsone 100–150 mg/day
-
Antimalarial drugs (eg, hydroxychloroquine)
-
Azathioprine 100–150 mg/day
- Others: thalidomide, cyclosporine, mycophenolate mofetil, photochemotherapy (PUVA)
What is the outlook for erythema multiforme?
Minor erythema multiforme usually resolves spontaneously without scarring for 2 to 3 weeks. Erythema multiforme major may take up to 6 weeks to resolve. Erythema multiforme does not progress to SJS/TEN.
There may be residual discoloration of mottled skin. Significant eye involvement in erythema multiforme major can rarely lead to serious problems, including blindness.
