What is cryoglobulinemia?
Cryoglobulinemia is a rare disorder characterized by the presence of abnormalities immunoglobulin proteins in the blood that can precipitate out in the tissues at low temperatures and causing inflammation and damages.
Immunoglobulins are the kind of proteins that make antibodies in response to foreign substances (antigens) introduced into the body. In cryoglobulinemia, abnormal immunoglobulins form complexes (cryoglobulins) and precipitate (leach) out of the blood at low temperatures. This causes restricted tissue blood flow and systemic inflammation, which leads to many clinical signs and symptoms, including skin lesions, arthralgia (joint pain), arthritis, vascular purple (purple skin marks), livedo (marbling pattern) and bleeding conditions.
Cryoglobulinemia often occurs in association with other diseases, particularly autoimmune or infectious diseases (this is known as secondary cryoglobulinemia). When it occurs without an associated disease, it is called idiopathic or essential cryoglobulinemia.
Types of cryoglobulinemia
Cryoglobulinemia is classified into 3 main types according to the composition of the cryoglobulin complex. Each type has been found to be associated with certain diseases.
| Cryoglobulin type | Immunoglobulin composition | Associated diseases |
|---|---|---|
| Type I: single monoclonal antibody | Mainly IgM Less frequently IgG and IgA |
Waldenström macroglobulinemia Chronic lymphocytic leukemia Multiple myeloma Lymphadenopathy Hairy Cell Leukemia |
| Type II: monoclonal rheumatoid factor mixed antibody (usually IgG or IgM) | IgM-IgG IgG-IgG IgA-IgG |
Waldenström macroglobulinemia |
| Type III: mixed antibody with rheumatoid polyclonal factor | IgM-IgG IgG-IgG-IgA |
Systemic lupus erythematosus |
Who gets cryoglobulinemia?
Cryoglobulinemia is believed to be rare. Essential mixed cryoglobulinemia occurs in about 1 in 100,000 people. Most cases of cryoglobulinemia have an underlying cause. The type of cryoglobulinemia found in patients is approximately 25% with type I, 25% with type II, and 50% with type III.
It tends to develop between 40 and 60 years of age and affects women more than men in 3: 1.
What are the clinical features of cryoglobulinemia?
The clinical characteristics of cryoglobulinemia differ between the types shown in the table below.
| Characteristics of type I cryoglobulinemia | Characteristics of type II and III cryoglobulinemia |
|---|---|
|
|
Cutaneous manifestations of cryoglobulinemia.
Skin problems are almost always present in patients with cryoglobulinemia.
| Skin problem | Type i (%) | Types II and III (%) |
|---|---|---|
| Ischemic necrosis (skin and tissue damage due to lack of blood flow) | 40 | 0-20 |
| Palpable purple | 15 | 80 |
| Livedoid vasculopathy | 1 | 14 (in type III) |
| Cold-induced urticaria | 15 | 10 (in type III) |
| Scarring of the tip of the nose, pinnae, fingers and toes. | ||
| Nail fold capillary abnormalities | ||
Cryoglobulinemia affecting the hands and feet.
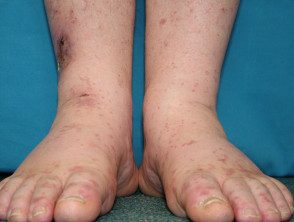
Cryoglobulinemia
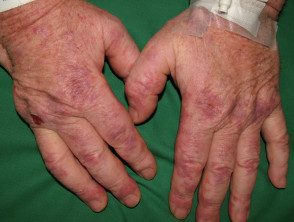
Cryoglobulinemia
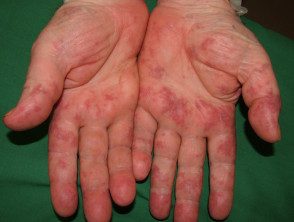
Cryoglobulinemia
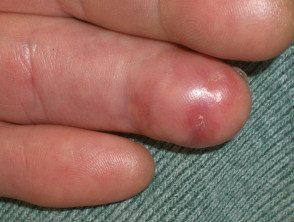
Cryoglobulinemia
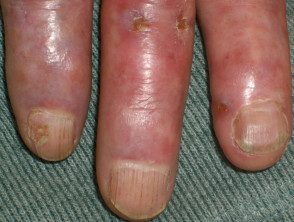
Cryoglobulinemia
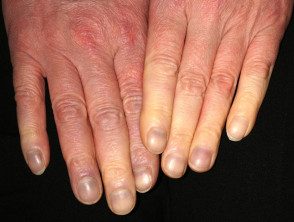
Raynaud's phenomenon
Other manifestations of cryoglobulinemia
Many organs can be affected by cryoglobulinemia.
| Organ affected | Signs and symptoms |
|---|---|
| Light | Cough, shortness of breath, fluid in the lungs. |
| Gastrointestinal | Stomach pain, bleeding, enlarged liver and / or spleen. |
| Kidneys | Hypertension (high blood pressure), glomerulonephritis, nephrotic syndrome |
| Nervous system | Visual disorders, peripheral neuropathy. |
Fever It can also happen.
What is the treatment for cryoglobulinemia?
The primary goal of therapy is to find and treat the underlying cause and to limit cryoglobulin precipitation and resulting inflammation. Cryoglobulinemia patients should be advised to avoid cold environments to avoid precipitation of cryoglobulins.
Symptomatic treatment includes:
- Nonsteroidal anti-steroidsinflammatory medications for arthralgia and fatigue.
- Immunosuppressive drugs (eg, corticosteroids, cyclophosphamide, azathioprine) when there is organ involvement such as vasculitis, kidney disease, progressive neurological symptoms and serious and disabling skin conditions.
- Plasmapheresis is used for serious or life-threatening complications.
- Antiviral The therapy is effective in patients with cryoglobulinemia associated with hepatitis C.
- The anti-CD20 monoclonal antibody rituximab has been reported to be effective in vasculitis due to mixed cryoglobulinemia type II and cryoglobulinemia associated with hepatitis C.
Identifying and treating early symptoms, such as skin lesions, fatigue, or arthralgia as a result of cryoglobulinemia, will prevent further organ damage and improve patient outcomes.

