What is it erythroderma?
Erythroderma is a generalized redness of the skin. It is a very serious skin condition that can be fatal. It may be the result of many inflammatory skin conditions, drugs and malignancies, but in one third of cases it is due to psoriasis.
Erythrodermic psoriasis
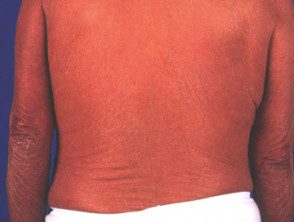
Erythrodermic psoriasis
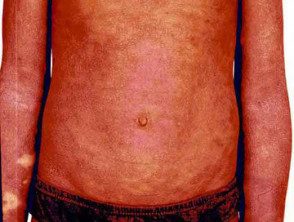
Erythrodermic psoriasis
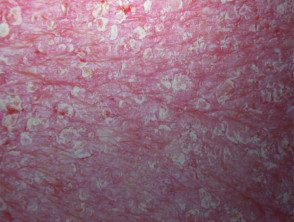
Erythrodermic psoriasis
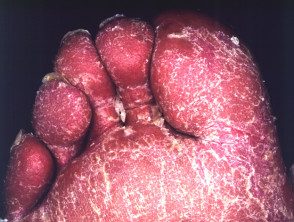
Erythrodermic psoriasis
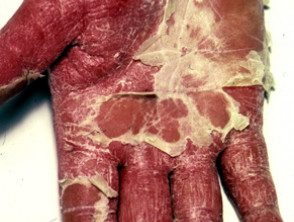
Erythrodermic psoriasis
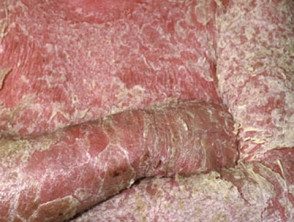
Erythrodermic psoriasis
What Causes Erythrodermic Psoriasis?
Erythrodermic psoriasis can be precipitate by:
- Infections
- Low in calcium
- Withdrawal of oral corticosteroids (prednisone)
- Withdrawal of excessive use of strong current corticosteroids
- Strong coal tar preparations
- Certain medications including lithium, antimalarials, and interleukin II
- Excessive alcohol consumption.
What are the clinical features of erythrodermic psoriasis?
Erythrodermic psoriasis usually occurs in the setting of known worsening or unstable psoriasis, but it can be the first presentation of psoriasis. Onset can occur acutely over a few days or weeks, or progress gradually over several months from pre-existing psoriasis.
The characteristics are those of any form of erythroderma (red and dry skin all over the body).
Complications include:
- Dehydration
- Heart failure
- Infection
- Hypothermia
- Protein loss and malnutrition.
- Edema (swelling), particularly of the legs
- Death
What is the treatment for erythrodermic psoriasis?
Treating erythrodermic psoriasis can be difficult. Management includes:
- Hospitalization for supportive care, including IV fluids and temperature regulation.
- Nice emollients and cool wet dressings
- Bed rest
- Treatment of complications (eg, antibiotics, diuretics (water tablets), nutritional support)
- Low-dose methotrexate, cyclosporine, or acitretin
- Individual cases have been reported to have successful results with biological agents, including the TNF-alpha inhibitors adalimumab, etanercept, and infliximab, and the IL12 / 23 inhibitor, ustekinumab.
Oral corticosteroids should be avoided if possible because withdrawal runs the risk of worsening erythrodermic status and may cause generalization pustular psoriasis. However, sometimes they are the only treatment that helps.
Topical tar preparations and phototherapy should also be avoided in the early treatment of erythrodermic psoriasis, as they can make the condition worse.

