What is xanthoma?
A xanthoma is a skin injury caused by the accumulation of fat in macrophage immune cells on the skin and more rarely in the layer of fat under the skin.
Some types of xanthoma are indicative of lipid metabolism disorders (for example, hyperlipidemia or high blood fats), where they may be associated with an increased risk of coronary heart disease and occasionally with pancreatitis.
Xanthomas are classified into the following types based on where they are in the body and how they develop.
Xantelasma palpebrum
- The most common type of xanthoma
- Lesions arise symmetrically on the upper and lower eyelids.
- The lesions are smooth, velvety, yellow, flat. papules or plates
- The lesions start as a small bump and gradually enlarge over several months.
- May or may not be associated with hyperlipidemia
See more images of xanthelasma.
Xanthelasma
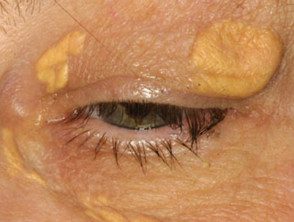
Xanthelasma
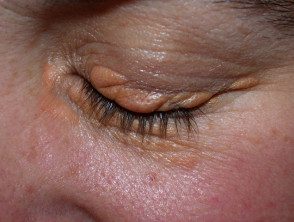
Xanthelasma
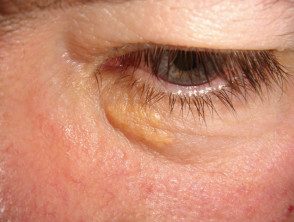
Xanthelasma
Tuberous xanthoma
- Firm, painless, red-yellow. nodules that develop around pressure areas, such as the knees, elbows, heels, and buttocks
- Lesions can join to form multilobed masses
- Usually associated with hypercholesterolemia (increased cholesterol blood levels) and increased LDL levels
Tuberous xanthoma
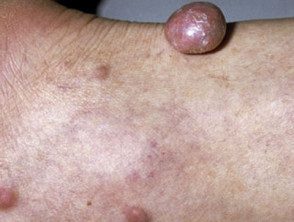
Tuberous xanthomas
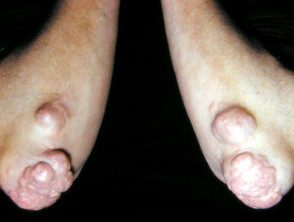
Tuberous xanthomas
Tendon xanthoma
- Appears as slow magnification subcutaneous nodules related to a tendon or ligament
- Most commonly found on the hands, feet, and Achilles tendon
- Associated with severe hypercholesterolemia and elevated LDL levels
Tendon xanthoma
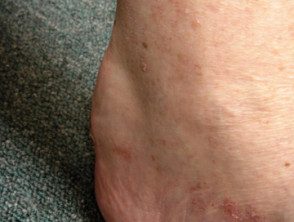
Tendon xanthoma
Eruptive xanthoma
- The lesions usually appear as small red-yellow papule cultures.
- Most often they arise on the buttocks, shoulders, arms and legs, but can appear throughout the body.
- Rarely, the face and the inside of the mouth can be affected.
- Lesions can be tender and usually itchy
- Lesions can resolve spontaneously in a few weeks.
- Associated with hypertriglyceridemia (increased triglycerides blood levels) often in patients with diabetes mellitus (sugar diabetes)
Eruptive xanthomas
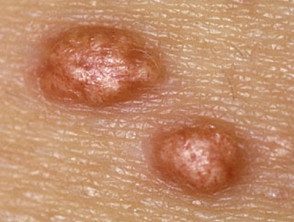
Eruptive xanthomas
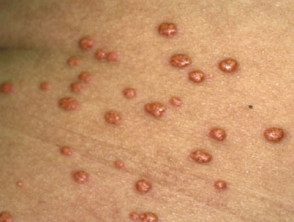
Eruptive xanthomas
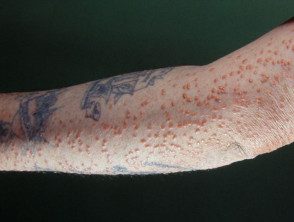
Eruptive xanthomas
Flat xanthoma
- Lesions are flat papules or patches that can appear anywhere on the body.
- Injuries to the folds of the palms are indicative of a specific pattern of increase lipids in the blood called dysbetalipoproteinemia type III
- May be associated with hyperlipidemia and hypertriglyceridemia
Diffuse flat xanthomatosis
- A rare form of histiocytosis.
- Associated with an abnormal antibody in the blood called a paraprotein.
- Lipid levels are normal.
- Around 50% will have a malignancy blood usually multiple myeloma or leukemia.
- It comes with large flat, reddish-yellow patches on the face, neck, chest, buttocks, and skin folds (such as the armpits and groin).
Xanthomas diffuse plane
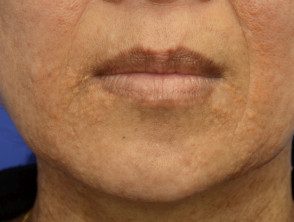
Xanthomas diffuse plane
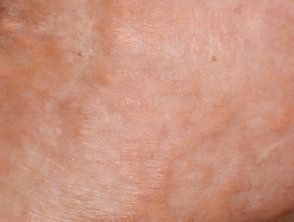
Xanthomas diffuse plane
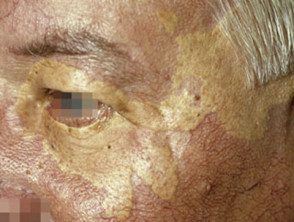
Xanthomas diffuse plane
Disseminated xanthoma
- Xanthoma-like lesions due to a rare form of histiocytosis.
- Lipid metabolism is normal.
- Skin lesions generally consist of hundreds of small yellowish-brown or reddish-brown bumps, which generally spread evenly on both sides of the face and trunk. They can particularly affect the armpits and groin.
- Small bumps can join together to form sheets of thickened skin.
- The 30% of affected people have involvement of the lining of the mouth, airways or eyes (mucous membrane surfaces). Warty Plaques in the mouth are called verruciform xanthomas.
- The 40% of affected people develop diabetes insipidus, a condition that results in the inability to control water loss (resulting in continuous thirst and excessive urine production). This is due to histiocyte overgrowth in the lining of the brain (meninges).
- It can affect internal organs (such as liver, lungs, kidneys, etc.)
- Self-limiting and eventually improves on its own, but can persist for many years.
Disseminated xanthoma
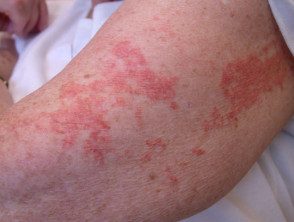
Disseminated xanthoma
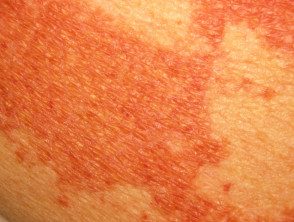
Disseminated xanthoma
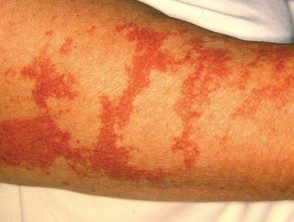
Disseminated xanthoma
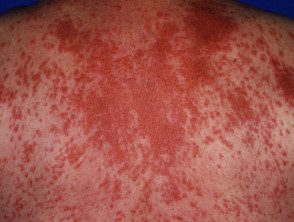
Disseminated xanthoma
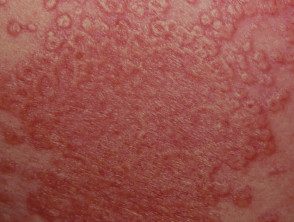
Disseminated xanthoma
What causes xanthoma?
There are several underlying disorders in which xanthoma is caused by an alteration in the metabolism of lipids (fats). Because lipids are insoluble in water, they combine with proteins to form compounds called lipoproteins. Lipoproteins transport lipids and cholesterol in the blood to different parts of the body. Depending on their size and weight, common lipoproteins are classified into chylomicrons, very low-density lipoproteins (VLDL), low-density lipoproteins (LDL), and high-density lipoproteins (HDL) (Fredrickson classification). Everyone has a role to play in maintaining the body's metabolic function.
Alterations in lipoproteins may be the result of a genetic defect (eg. primary hyperlipoproteinemia) or some underlying systemic disorder like diabetes mellitus, hypothyroidismor nephrotic syndrome. These underlying diseases can cause elevated levels of certain lipids and lipoproteins, which then manifest as cutaneous xanthoma
Monogenic family hypercholesterolemia: type IIa
- Mutation in the LDL receiver
- High LDL levels
- Total cholesterol in heterozygotes 9–14 mmol / L
- Total cholesterol in homozygotes 15-30 mmol / L
Familial polygenic hypercholesterolemia: type IIa
- Mixed genetic and lifestyle causes
- Wide range of results
Polygenic Familial Combined Hyperlipidemia: Type IIb
- Mixed genetic and lifestyle causes
- High total cholesterol
- High triglycerides
- Low HDL cholesterol
- Increased VLDL cholesterol
- LDL may be normal but denser and more likely to cause atheroma
Moderate hypertriglyceridaemia
- It is also often associated with high blood pressure, obesity, diabetes mellitus, metabolic syndrome, high insulin levels, high uric acid levels
- May be due to alcohol or medications like systemic steroids, isotretinoin, acitretin
- Triglycerides 2_10 mmol / L
- Often associated with low HDL cholesterol
Severe hypertriglyceridemia: type 1 and V
- Mixed genetic and lifestyle causes
- Mellitus diabetes
- Familial LPL deficiency
- Triglycerides> 10 mmol / L
- High total cholesterol
- Elevated chylomicrons
- High VLDL cholesterol
Wide beta hyperlipoproteinemia: type III
- Rare apo E gene mutation
- Triglycerides 5–20 mmol / L
- Total cholesterol 7–12 mmol / L
The reason for the appearance of xanthoma when fats in the blood are normal is not understood at this time.
What evaluation is required for xanthoma?
A skin biopsy It may be necessary to confirm a clinical diagnosis of xanthoma. See eruptive xanthoma pathology.
Appropriate blood and urine tests and x-rays are done to determine the cause of the altered lipoprotein levels if they are present. The risk of cardiovascular disease, including heart attacks, peripheral vascular disease and stroke, increases with elevated levels of certain lipoproteins. Identifying contributing factors is essential for proper therapy to be established.
What is the treatment for xanthoma?
The primary goal of treating xanthoma associated with an underlying lipid disorder is to identify and treat the lipid disorder. In many cases, treatment of the underlying disorder will reduce or resolve xanthoma. Additionally, treating hyperlipidemia will reduce the risk of heart disease, and treating hypertriglyceridemia will prevent pancreatitis. Diet and lifestyle modifications with or without medications are used to treat lipid disorders.
Dietary measures should include:
- Prepare most meals from vegetables, salads, cereals, and fish.
- Minimize saturated fats (found in meat, butter, other dairy products, coconut oil, palm oil)
- Minimize your intake of simple and refined sugars found in soda, candy, cookies, and cakes.
- If you are obese or overweight, try to reduce your weight slowly by reducing calorie intake and increasing exercise.
Very effective medications can also be prescribed. These may include:
- Statins (HMG CoA reductase inhibitors), such as simvastatin and atorvastatin, reduce cholesterol production in the liver, resulting in lower LDL cholesterol levels, increase HDL cholesterol, and slightly lower triglycerides. Treatment should be controlled by regular blood tests to check lipid levels and to secure the liver and muscles. enzymes They are normal, since statins sometimes cause abnormalities, especially when prescribed in higher doses.
- Fibrates, such as bezafibrate, can be added to reduce the production of triglycerides in the liver, decrease triglycerides, and increase HDL cholesterol. They can cause gastrointestinal side effects.
- Ezetimibe can be added in high-risk patients or if higher statin doses are poorly tolerated. Reduces the absorption of cholesterol from the intestine, lowering total cholesterol and LDL.
- Nicotinic acid lowers cholesterol, LDL cholesterol, and triglycerides, and increases HDL cholesterol. TO therapeutic dose of at least one gram a day, causes redness. A analog term, acipimox, is better tolerated.
- Cholestyramine and colestipol are rarely used as they are not as effective as the medications listed above and are poorly tolerated.
Surgery or locally destructive modalities can be used to remove xanthomas that do not resolve spontaneously or with treatment of the underlying cause. Disseminated xanthoma that affects the functions of vital organs can be treated by chemotherapy drugs or radiotherapy.
Xanthelasma treatments include:
- Current trichloroacetic acid (see chemical peels)
- Electrodesiccation
- Cryotherapy
- To be vaporization (eg Nd: YAG, Er: YAG and Q-switched carbon dioxide)
- Excision.
Intralesional bleomycin injection has been used successfully off-label.
Trichloroacetic acid treatment of xanthelasma
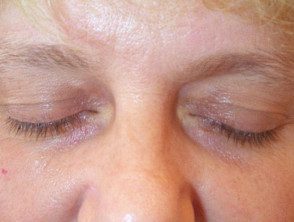
One month after
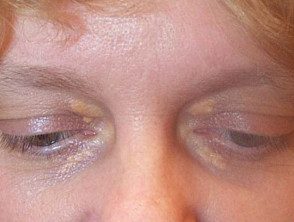
Before treatment
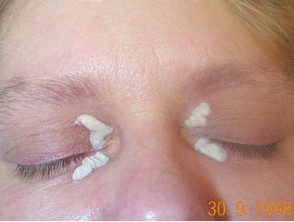
During treatment

