What is it erosive lichen planus?
Erosive lichen planus is a chronic and painful condition affecting mucous membrane surfaces, mainly the mouth (oral lichen planus) and the genitalia (vulvar or penile lichen planus).
A severe variant or erosive lichen planus in women is known as vulvovaginal gingival syndrome. Ulceration occurs in the mouth and gums as well as in the vulva and in the vagina Peningingival syndrome is the equivalent condition in men.
Erosive lichen planus is sometimes associated with classic cutaneous lichen planus or other forms of lichen planus of the mucosa.
Who gets erosive lichen planus?
Erosive lichen planus most often affects people between the ages of 40 and 70. It is at least twice as common in women as in men.
What causes erosive lichen planus?
Erosive lichen planus is a destructive autoimmune disease of unknown cause involving T lymphocytes.
- Occasionally, it is drug induced and will resolve by removing the responsible drug.
- The partial response to antifungals and antibiotics indicates that an abnormal response to the local microflora may be involved, especially Candida albicans.
- Cytokine the expression profile has found higher levels of interleukins, IL 17 and IL 23.
What are the clinical characteristics of erosive lichen planus?
Erosive lichen planus causes pain and persistence ulcers. These heal with scars. It mainly affects adults, particularly women, and is rare in children.
Oral erosive lichen planus
In the mouth, erosions and ulcers may be the only signs (ulcerative stomatitis) They can occur inside the cheeks, on the sides of the tongue, on the gums or inside the lips. Unlike short-lived aphthous ulcers, erosive lesions of lichen planus are larger and more irregular, and may persist for weeks or longer. Eating can be very painful, resulting in weight loss, nutritional deficiencies, and depression.
Other forms of oral lichen planus may also be present, such as white lace streaks and inflammation and desquamation of the gums (desquamative gingivitis).
Oral erosive lichen planus
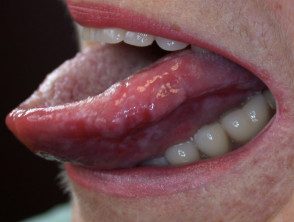
Erosive oral lichen planus
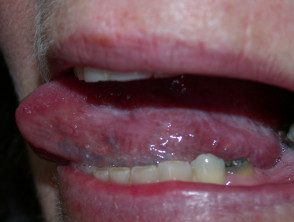
Erosive oral lichen planus
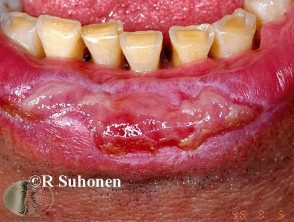
Erosive oral lichen planus
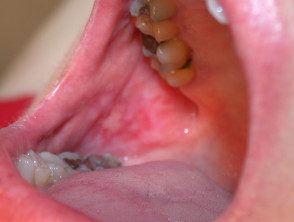
Erosive oral lichen planus
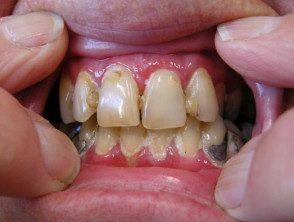
Erosive oral lichen planus
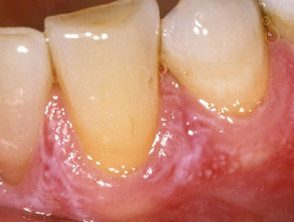
Erosive oral lichen planus
Genital erosive lichen planus
In women, erosive lichen planus affects the labia minora (inner lips) and the introitus (entrance to the vagina). The affected mucous membrane It is bright red and raw. Erosive lichen planus can be very painful, itching when urinating and avoiding sexual intercourse. It is a cause of vulvodynia (burning vulva discomfort). Erosive lichen planus can also cause very severe itching.
The hood of the clitoris may disappear, and the labia minora may shrink and adhere to each other or to the labia majora (the outer lips). also can scar, closing on the vagina.
Sometimes, erosive lichen planus affects deep within the vagina, where it causes inflammation and superficial ulceration (desquamative vaginitis). Cells on the surface of the vagina break loose and cause mucus. download. The eroded vagina can easily bleed on contact.
Erosive lichen planus in men affects the end of the penis (the glans), which becomes red, raw, and tender.
Images of erosive lichen planus affecting the vulva
Other mucosa sites
Erosive lichen planus rarely affects the eyelids, the external ear canal, the esophagus, larynx, bladder and anus.
What is the cause of erosive lichen planus?
The cause or causes of erosive lichen planus are unknown. It is considered an autoimmune disease, where immune cells called T lymphocytes attack the epidermal cells from affected areas.
Erosive lichen planus is not due to infection or allergy.
Erosive lichen planus complications
Infections
Patients with erosive lichen planus can develop infections particularly Candida albicansHerpes simplex, Staphylococcus aureus. Herpes infections are particularly painful and can cause vulvar ulceration.
Scaly cell carcinoma
In about 1-3% cases, longstanding erosive lichen planus can cause Cancer (squamous cell carcinoma, SCC) of the mouth (oral cancer), vulva (vulva cancer), and penis (penile cancer). This should be suspected if there is an enlarged lump or a ulcer with thickened edges.
Some patients with erosive lichen planus have a particularly high risk of SCC:
- Smokers
- Immunosuppressed patients due to illness or drugs.
- Patients infected with oncogenic types of human papillomavirus (HPV, see genital warts).
Scars
Erosive lichen planus is a destructive disorder. Even when the inflammatory The component has resolved, scars can interfere with eating or sexual function.
How is erosive lichen planus diagnosed?
The diagnosis of erosive lichen planus is often made by typical history and clinical appearance. A biopsy It may be recommended to confirm the diagnosis and look for cancer. Histopathological signs of a 'lichenoid tissue reaction that affects the epidermis (the layer of skin cells) are supportive.
However, the ulcerative nature of the disorder means that the epidermis may be missing, so lichenoid features may not be observed. the pathologist can describe a rapid inflammatory infiltrate in the mucosa, but this is not specific.
Direct immunofluorescent staining of tissue may also be helpful.
What is the treatment of erosive lichen planus?
Management of erosive lichen planus can be very challenging. Since it is a chronic complaint, current and systemic Treatment may be necessary intermittently or continuously, in the long term.
General measures
For oral disease, it is important to practice good oral hygiene and get regular dental checkups. Avoid foods that hurt your mouth.
The genitals should be gently washed with water alone or with a soap-free cleanser, such as an aqueous solution. cream. A non-irritating emollient such as petroleum jelly can be applied as desired.
Ultra Powerful Topical Steroids
Topical steroids are generally applied daily for courses of 4 to 6 weeks. They are the basis of therapy in most patients, but maintenance treatment 1-3 times per week or more frequently may be necessary in the long term.
- In the mouth, topical steroids can be supplied as a pastenasal spray (intended for rhinitis) or the preventive smoker of asthma. These should be applied to the eroded areas two or three times a day.
- For genital erosions, ultra powerful steroids ointment (eg, clobetasol propionate) should be applied to the affected area as a thin sample once a day. Cream may be preferred, but is more likely to sting when applied.
- Hydrocortisone foam can be used inside the vagina or anus.
Calcineurin inhibitors
Calcineurin inhibitors, such as pimecrolimus cream or tacrolimus ointment, have been shown to be very effective for some patients with erosive lichen planus. These are applied once or twice a day for several weeks. The treatment can be repeated as necessary.
Mouthwashes containing cyclosporine or tacrolimus have been found to help oral disease.
Systemic steroids
Systemic steroids, such as prednisone, can be prescribed for a few weeks or more, generally at a dose of 0.5 to 1 mg / kg / day. Once the erosions have healed, the dose is reduced. Long-term use of systemic steroids can have serious side effects. In many patients, calcium and vitamin D should also be prescribed to reduce the chance of corticosteroid-induced bone thinning.
Methotrexate
Methotrexate is taken in a dose of 10-20 mg once a week. Folic acid is often added to reduce the chance of possible side effects. This can be very effective for erosive lichen planus, with improvement or healing occurring within one to three months. It can be continued in the long term if necessary. Blood count, liver function, and procollagen levels should be monitored. Alcohol consumption should be minimized. It should not be taken during pregnancy.
Other oral treatments
Other medications that sometimes help include:
- Mycophenolate mofetil
- Oral antibiotics, such as a tetracycline
- Oral antifungal agents
- Acitretin
- Hydroxychloroquine
- Azathioprine
- Cyclosporine
- Dapsone
- Colchicine
- Thalidomide
Surgery
Surgical release of vulvar and vaginal adhesions and healing of lichen planus may be performed occasionally to reduce urination difficulties and allow intercourse. Procedures may include:
- Vaginal dilation
- Simple perineotomy (division of adhesions)
- Fenton procedure (a incision that is repaired transversely)
- Perineoplastyexcision of involved tissue and advancement of the vaginal mucosa)
Other treatments that have been tried include photodynamic therapy and focused ultrasound therapy.

