What is it acute rheumatic fever?
Acute rheumatic fever (ARF) is caused by a reaction to a bacterial infection with particular strains of group A streptococci. It was long thought that ARF only follows streptococci pharyngitis (sore throat), however recent studies of Aboriginal populations in Australia have suggested that streptococcal infection of the skin may precede some cases of ARF. Those who have experienced an episode of ARF are more likely to suffer recurrent subsequent attacks with group A streptococcal infections.
The skin sign of acute rheumatic fever is erythema marginatum.
Who gets rheumatic fever?
ARF generally affects children ages 5 to 15. Most ARI cases currently occur in developing countries. There are an estimated 470,000 new cases of ARF a year worldwide (60% of which eventually develop rheumatic heart disease). In most developed countries, ARF is now rare, with a few notable exceptions; The highest documented rates of ARI in the world are found in Maori and Pacific in New Zealand, Aboriginal Australians, and those in Pacific Island nations.
Rheumatic fever is associated with poverty, overcrowding, and poor sanitation facilities. It is suspected that there genes that make some families more susceptible to the disease.
What are the clinical features of acute rheumatic fever?
Symptoms of ARF usually develop several weeks after an episode of strep throat. However, many patients do not recall having a sore throat. Non-specific symptoms include:
- Fever
- Abdominal pain
- Muscle pains
ARF causes a variety of more specific clinical features:
- Polyarthritis (multiple swollen joints) - most often ankles, knees, elbows, wrists. Arthritis it can migrate from one joint to another.
- Carditisinflammation heart): involves the heart valves, the heart muscle, and the membrane that surrounds the heart.
- Sydenham chorea: it is a disorder of the nervous system characterized by personality changes, muscle weakness and involuntary movements.
Skin signs in ARF can include:
- Rheumatic marginal erythema: this is a characteristic kind of cancel erythema occurring in approximately 10% of the first ARF attacks in children; It is very rare in adults. the eruption It can be difficult to detect in dark-skinned people. When present, it is found on the trunk and upper arms and legs, but rarely on the face, palms, or soles. The rash appears pink or red macules (flat spots) or papules (small lumps), which extend outward in a circular fashion. As the lesions progress, the edges become raised and red, and the center clears. The lesions are not itchy or painful, and are sometimes unnoticed by the patient. Lesions can disappear and reappear within hours, reappearing in hot conditions. Erythema marginate can persist intermittently for weeks or months, even after successful ARF treatment.
- Subcutaneous nodules (small lumps under the skin): these are rare and occur in less than 2% of patients with ARF. Painless nodules are found over the joints (such as the elbows, knees, ankles, and knuckles), the back of the scalp, and the vertebrae (spine). The nodules are firm, round, mobile, and 0.5-2 cm in size. Nodules are usually only found when there is severe carditis. They usually resolve within a month, but they can persist longer.
Marginal erythema
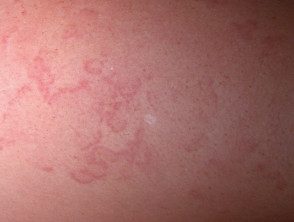
Marginal erythema
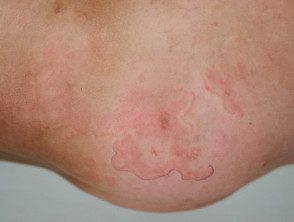
Marginal erythema
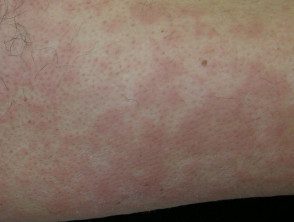
Marginal erythema
What are the complications of acute rheumatic fever?
The most serious complication of recurrent ARF is permanent damage to the heart valves, known as rheumatic heart disease. The disease can cause permanent damage to:
- Heart valves, particularly the mitral valve and aortic valve, which can lead to valvular stenosis and / or regurgitation.
- Heart muscles, reducing the pumping action, that is, causing heart failure.
- The membrane around the heart, causing pericarditis.
- Irregular heart rhythms, such as atrial fibrillation.
How is acute rheumatic fever diagnosed?
The diagnosis of ARF is challenging, as there are no clinical features or diagnostic tests available to confirm or rule out this condition. Instead, the diagnosis is made using the Jones criteria. These criteria require evidence of a preceding group A streptococcal infection, and various combinations of the above characteristic features and other nonspecific clinical features. A detailed explanation of these criteria (and modifications for the New Zealand environment) can be found on the website of the National Heart Foundation of New Zealand.
Tests to confirm evidence of a group A streptococcal infection include:
- Blood tests to detect elevation or elevation antibodies to group A streptococcus. The most commonly used tests are plasma antistreptolysin O and antideoxyribonuclease B titers.
- Culture of throat swabs and fast antigen The tests for group A strep are less accurate.
Other tests used in the evaluation of a patient with suspected ARF include:
- Blood tests: markers of inflammation, such as ESR or CRP, can be elevated
- Electrocardiogram and echocardiogram to identify cardiac involvement
- Doppler and color flow mapping to detect minor valve defects not clinically evident
What is the treatment for rheumatic fever?
Following a diagnosis of rheumatic fever, it is standard practice to treat the group A streptococcal infection that led to the disease with oral penicillin (although this practice has not been shown to alter long-term outcomes).
After the initial attack, patients are treated with continuous penicillin to prevent further streptococcal colonization or infection and further damage to the heart. Continuous penicillin is also recommended for people with established rheumatic heart disease. Continuous penicillin is usually given by injection every four weeks for a minimum of 10 years. Some patients, such as those with severe carditis, may require lifelong treatment.
Aspirin or naproxen are added to reduce inflammation, fever, and pain. In extreme cases, a corticosteroid such as prednisone can be added.
Sometimes, patients with rheumatic heart disease may require heart surgery to repair or replace damaged heart valves.
Can rheumatic fever be prevented?
ARF can be prevented with prompt treatment of group A strep throat, particularly in people 5 to 15 years of age. People with a sore throat and fever should see a doctor. Vaccines are currently being developed and eagerly awaited.

