What is it venous eczema?
Venous Eczema is a Common Form of Eczema /dermatitis affecting one or both legs in association with venous insufficiency. Also called gravitational dermatitis.
Who Gets Venous Eczema?
Venous eczema is seen more frequently in middle-aged and elderly patients; It is reported to affect 20% of those over 70 years of age. Is associated with:
- History of deep veins thrombosis on an affected limb
- History of cellulite on an affected limb.
- Chronic lower leg swelling, aggravated by hot weather and prolonged standing
- Varicose veins
-
Venous leg ulcers.
What Causes Venous Eczema?
Venous eczema appears to be due to the accumulation of fluid in the tissues and the activation of the innate immune response.
Normally when walking, the leg muscles pump blood upward and valves in the veins prevent pooling. A clot in the deep veins of the legs (deep vein thrombosis or DVT) or varicose veins can damage the valves. As a result, a back pressure develops and fluid builds up in the tissues. A inflammatory the reaction occurs
What are the clinical features of venous eczema?
Venous eczema can form discreet patches or become confluent and circumferential. Features include:
- Red itchiness, blisters and scabs plates; or dry cracked and scaly plates on one or both legs
- Orange brown macular pigmentation because hemosmosin statement
- Atrophie blanche (irregular white scars surrounded by red spots)
- 'Champagne bottle' shape at the lower leg: tapering at the ankles and hardening (lipodermatosclerosis)
Venous disease
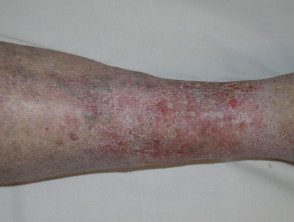
Venous eczema
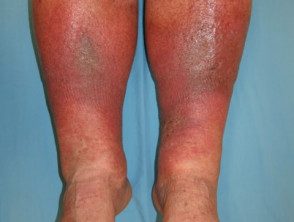
Lipodermatosclerosis
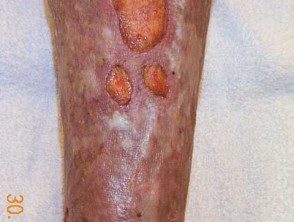
Venous ulcer
What are the complications of venous eczema?
- Impetiginization - secondary infection with Staphylococcus aureus resulting in yellowish scabs
-
Cellulitis - infection with Streptococcus pyogenes: there may be redness, swelling, pain, fever, a red streak on the leg and swollen glands in the groin
-
Secondary eczema: Eczema spreads to other areas of the body.
-
Contact allergy to one or more components of the ointments or creams used
How is venous eczema diagnosed?
The diagnosis of venous eczema is clinical.
Patch Tests may be done if there is a suspected contact allergy.
What is the treatment for venous eczema?
Reduces swelling in the leg
- Don't stand for long periods.
- Take regular walks.
- Elevate your feet when sitting - If your legs are swollen, they must be above your hips to drain effectively.
- Elevate the feet of your bed at night.
- During the acute eczema phase, bandaging is important to reduce swelling.
- When the eczema has settled, wear graduated compression stockings or long-term stockings. Tight-fitting moderate to high compression socks can be obtained from a surgical supply company. Light compression with travel socks may be adequate, and they are easy to put on. They can be bought in pharmacies, travel and sports stores. More compression is obtained using two pairs.
-
Horse chestnut extract appears to be beneficial for at least some patients with venous disease.
Treat eczema
- Dry the patches that ooze with Condy's solution (potassium permanganate) or vinegar diluted in gauze as compresses.
- Oral antibiotics such as flucloxacillin may be prescribed for a secondary infection.
- Apply a prescribed current steroid: start with a powerful steroid cream Precisely applied daily to patches until flattened. After a few days, switch to a milder steroid cream (eg, Hydrocortisone) until the itchy patches have resolved (maintenance treatment). Check with your doctor if you are using steroid creams for more than a few weeks. Overuse can thin the skin, but short courses of stronger preparations can be used from time to time if necessary to control dermatitis. Coal tar ointment It can also help.
- Use a moisturizer frequently to keep the skin on your legs smooth and soft. If the skin is very scaly, urea cream can be especially effective.
- Protect your skin from injury - this can lead to infection or ulceration that can be difficult to cure.
Treatment for varicose veins
- Seek the opinion of a vascular varicose vein surgeon
- These can be treated surgically, for intravenous To beor sclerotherapy.
- Varicose veins can develop again after an apparently successful operation because venous disease is progressive.
How can venous eczema be prevented?
Venous eczema cannot be completely prevented, but the number and severity of flare-ups can be reduced with the following measures.
- Avoid standing or sitting for a long time with your legs down
- Wear compression stockings or stockings.
- Avoid and treat leg swelling.
- Apply emollients frequently and regularly to dry the skin
- Avoid soap; use plain water or soap-free cleansers when bathing
What is the prognosis for venous eczema?
Venous eczema tends to be a lifelong recurrent or chronic disorder. Try reappearance promptly with topical steroids.

