What is it hyperhidrosis?
Hyperhidrosis is the name given to excessive and uncontrollable sweating.
Sweat is a weak salt. solution produced by the eccrine sweat glands. These are distributed throughout the body, but are most numerous on the palms and soles (with approximately 700 glands per square centimeter).
Hyperhidrosis of palms and soles.
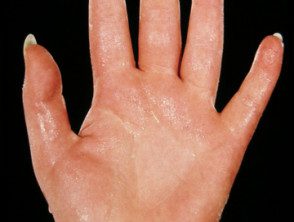
hyperhidrosis
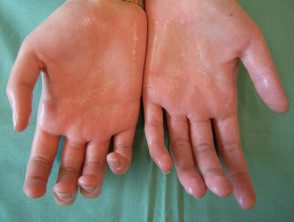

Who gets hyperhidrosis?
Primary Hyperhidrosis is reported to affect 1–3% of the US population and almost always begins during childhood or adolescence. The tendency may be inherited, and is reported to be particularly predominant in the japanese
Secondary hyperhidrosis is less common and can occur at any age.
What causes hyperhidrosis?
Primary hyperhidrosis appears to be due to hyperactivity of the hypothalamic thermoregulatory center in the brain and is transmitted through the sympathetic nervous system to the eccrine sweat gland.
Triggers for sweating attacks can include:
- hot weather
- Exercise
- Fever
- Anxiety
- The spicy food
secondary causes located Hyperhidrosis includes:
- The auriculotemporal syndrome (gustatory hyperhidrosis)
- Race
- spinal nerve damage
- Peripheral nerve damage, when it may be associated with cutaneous dysesthesia
- Surgical sympathectomy
- Neuropathy
- A brain tumor
- Chronic anxiety disorder
secondary causes generalized Hyperhidrosis includes:
- Obesity
- Diabetes
- Menopause
- overactive thyroid
- cardiovascular disorders
- Respiratory insufficiency
- Other endocrine tumors, such as pheochromocytoma
- Parkinson's disease
- Hodgkin lymphoma
Drugs: alcohol, caffeine, corticosteroids, cholinesterase inhibitors, tricyclic antidepressants, selective serotonin reuptake inhibitors, nicotinamide, and opioids.
What are the clinical features of hyperhidrosis?
Hyperhidrosis can be localized or generalized.
- Localized hyperhidrosis affects the armpits, palms, soles, face, or other sites.
- Generalized hyperhidrosis affects most or all of the body.
It can be primary or secondary.
primary hyperhidrosis
- It begins in childhood or adolescence.
- It may persist throughout life or improve with age.
- There may be a family history
- Tends to involve armpits, palms, and/or soles symmetrically
- Sweating usually reduces at night and disappears during sleep.
Secondary hyperhidrosis
- Less common than primary hyperhidrosis
- It is more likely to be unilateral and asymmetricor generalized
- It can occur at night or during sleep.
- Due to endocrine or neurological conditions or drugs
What is the impact of excessive sweating?
Hyperhidrosis is embarrassing and interferes with many daily activities.
Axillary hyperhidrosis
- Clothes get wet, stain and need to be changed several times a day.
- Moist skin folds are prone to irritation, irritating dermatitis and infection
Axillary hyperhidrosis

Palm hyperhidrosis
- Slippery hands prevent handshake.
- Marks left on paper and fabrics
- Difficulty writing perfectly
- Malfunction of electronic equipment such as keyboards and trackpads
- Prone to a blistering type of hand dermatitis (pompholyx)
Plant hyperhidrosis
- It affects the soles of the feet.
- Unpleasant smell
- ruined footwear
- Prone to a type of bullous dermatitis (pompholyx)
- Prone to secondary infection (tinea pedis, boneless keratolysis)
How is hyperhidrosis diagnosed?
Hyperhidrosis is usually diagnosed clinically. Testing is related to the possible underlying cause of hyperhidrosis and is rarely necessary for primary hyperhidrosis.
The precise site of localized hyperhidrosis can be revealed using the Minor test.
- Iodine (orange) is painted onto the skin and air dried.
- The starch (white) is sprinkled on top of the iodine.
- Sweating is revealed by a dark blue/black color change.
Screening tests for secondary generalized hyperhidrosis depend on other clinical features, but should include at a minimum:
- Blood sugar / glycosylated hemoglobin
- Thyroid function
What is the treatment of hyperhidrosis?
General measures
- Wear loose-fitting, stain-resistant, sweat-proof clothing.
- Change clothing and shoes when wet.
- Socks that contain silver or copper reduce infection and odor.
- Use absorbent inserts in shoes and replace them often.
- Use a soap-free cleanser.
- Apply corn starch dust after bath.
- Avoid foods and drinks with caffeine.
- Discontinue any medications that may be causing hyperhidrosis.
- Apply antiperspirant.
Current antiperspirants
- Deodorants are fragrances or antiseptics to disguise unpleasant odors; By themselves, they do not reduce perspiration.
Antiperspirants contain 10-25% aluminum salts to reduce sweating; “Clinical strength” aluminum zirconium salts are more effective than aluminum chloride.
- Topical anticholinergics such as glycopyrrolate and oxybutynin. gel have been successful in reducing sweating; Wipes containing glycopyrronium tosylate (Qbrexza™) were approved by the FDA in July 2018 for axillary hyperhidrosis in adults and children 9 years of age and older. Powder is available that contains the anticholinergic drug, 2% diphemanil.
- Antiperspirants are available as creamaerosol spray, stick, roll-on, wipe, powder and paint.
- Specific products are available for different body sites, such as armpits, other skin folds, face, hands and feet.
- They are best applied when the skin is dry, after a cold shower just before bed.
- Wash in the morning if it tends to irritate.
- Use once a week to daily if needed.
- If irritating, apply short-term hydrocortisone cream.
Iontophoresis
Iontophoresis is used for hyperhidrosis of the palms, soles and armpits.
- Main and battery powered units are available.
- The affected area is immersed in water or, with a more significant effect, in glycopyrronium solution.
- A mild electrical current is passed through the surface of the skin for 10-20 minutes.
- Repeated daily for several weeks, then less frequently as needed
- Iontophoresis may cause discomfort, irritation, or irritant contact dermatitis.
- Treatment requires a long-term commitment.
- It is not always effective.
Oral medications
Oral anticholinergic drugs
- Available medications are propantheline 15 to 30 mg up to three times daily, oxybutynin 2.5 to 7.5 mg daily, benztropine, glycopyrrolate (unapproved).
- They can cause dry mouth and, less commonly, blurred vision, constipation, dizziness, palpitations, and other side effects.
- People with glaucoma or urinary retention should not take them.
- Caution in elderly patients: an increased risk of side effects, including dementia, is reported.
- Oral anticholinergics can interact with other medications.
Beta blockers
- Beta blockers block the physical effects of anxiety.
- They can aggravate asthma or peripheral symptoms. vascular disease.
Calcium channel blockers, alpha-adrenergic agonists (clonidine) non-steroidal anti-steroidsinflammatory Drugs and anxiolytics may also be helpful for some patients.
Botulinum toxin injections
Botulinum toxin injections are approved for hyperhidrosis affecting the armpits.
- The injections reduce or stop sweating for three to six months.
- Botulinum toxins they are used without a license for localized hyperhidrosis in other sites, such as the palms.
- Botulinum toxin topical gel is under investigation for hyperhidrosis.
Surgical removal of the axillary sweat glands.
Overactive sweat glands in the armpits can be removed by various methods, usually under anesthetic.
- Tumescent liposuction (suctioning them out)
- Subcutaneous curettage (scrape them)
- Microwave thermolysis (the MiraDry® system approved by the FDA in 2011)
- Subdermal Nd:YAG To be
- High intensity microfocus ultrasound (experimental)
- Surgery to cut the skin of the armpits with sweat glands. If a large area needs to be removed, it can be repaired with a skin graft
Sympathectomy
Sympathetic spinal division. nerves by chemical or surgical endoscopic Thoracic sympathectomy (TSD) can reduce facial sweating (T2 ganglion) or armpit and hand (T3 or T4 node) but is reserved for the most severely affected people due to possible risks and complications.
- Hyperhidrosis can recur in up to 15% cases.
- Sympathectomy is often accompanied by undesirable warmth and dryness of the skin.
- New-onset hyperhidrosis of other sites occurs in 50 to 90% patients and is severe in 2%. It is reported to be less common after T4 ganglion sympathectomy compared to T2 ganglion sympathectomy.
- Serious complications include Horner's syndrome, pneumothorax (in up to 10%), pneumonia, and persistent pain (in less than 2%).
Lumbar sympathectomy is not recommended for hyperhidrosis affecting the feet, as it may interfere with sexual function.
What is the prognosis for hyperhidrosis?
Localized primary hyperhidrosis tends to improve with age. The prognosis for localized or generalized secondary hyperhidrosis depends on the cause.
Future treatments for hyperhidrosis.
Several research projects are underway to find safer and more effective treatments for hyperhidrosis. These include:
- DRM04 topical anticholinergic
- Combination of oxybutynin and pilocarpine (to counteract the adverse effects of the anticholinergic, oxybutynin) THVD-102

