What is multicentric reticulohistiocytosis?
Multicentric reticulohistiocytosis is very rare. systemic granulomatous disease classified as reticulocytosis and proliferative non-Langerhans cell histiocytosis. Multicentric reticulohistiocytosis is characterized by skin and mucous membrane injuries and arthritis [1].
Multicentric reticulohistiocytosis is known as lipoid dermatoarthritis, lipoid rheumatism, and giant cell reticulohistiocytosis.
Multicentric histiocytosis.
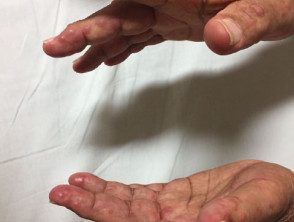
Multicentric histiocytosis.
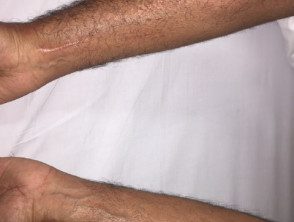
Multicentric histiocytosis.
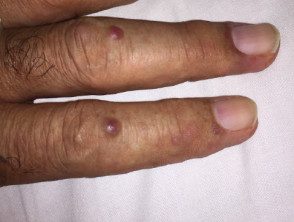
Multicentric histiocytosis.
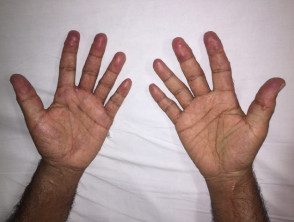
Multicentric histiocytosis.
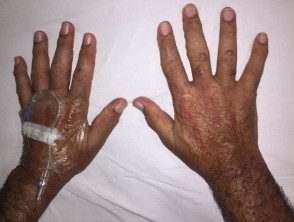
Multicentric histiocytosis.
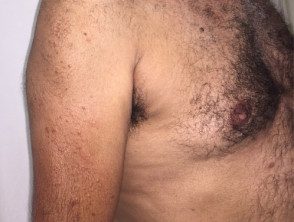
Multicentric histiocytosis.
Who gets multicentric reticulohistiocytosis?
Multicentric reticulohistiocytosis is more common in women than in men, with a ratio of 3: 1 [1]. The mean age of people affected by multicentric reticulohistiocytosis is 50 years. [2].
In approximately 1 in 4 cases, multicentric reticulohistiocytosis is associated with a malignancy [1]. The most common malignant neoplasms associated with multicentric reticulohistiocytosis are carcinomas of the lung, stomach, breast, cervix, colon, and ovary.
What Causes Multicentric Reticulohistiocytosis?
The cause of multicentric reticulohistiocytosis is unknown. If multicentric reticulohistiocytosis is a true paraneoplastic Clutter is controversial.
- Cancer it is unlikely if there are multiple skin lesions and there is no arthritis.
- No consistent type of cancer has been associated with multicentric reticulohistiocytosis.
- Because multicentric reticulohistiocytosis is very rare, the association with cancer may be coincidental.
- A correlation between cancer clearance and disappearance or improvement of multicentric reticulohistiocytosis has not been established.
Multicentric reticulohistiocytosis is also associated with:
- Vasculitis
- Autoimmune diseases like Sjogren syndrome and primary bile cirrhosis [3]
- Hyperlipidemia
What are the clinical features of multicentric reticulohistiocytosis?
Multicentric reticulohistiocytosis results in papules, nodules, and severe and rapidly destructive arthritis. It can affect the bones, tendons, muscles, joints, and solitary organs (eg, thyroid, eyes, lungs, kidneys, and liver) [1].
- In half of the patients, the first sign of the disease is arthritis.
- In a quarter, papules and nodules are the first sign.
- The rest develop skin and joint manifestations at the same time.
Arthritis
Arthritis most often involves the fingers, hands, knees, and shoulders, but any joint can be affected. Symptoms of arthritis can increase and decrease, but can quickly become severe and lead to joint destruction and deformity in approximately 45% of patients.
Cutaneous features
Multicentric reticulohistiocytosis skin lesions occur most frequently on the upper half of the body, especially on the face, ears, mucosal surfaces (lips, tongue, gums, nostrils, throat, eyelids), hands, and forearms.
- There are skin-colored or reddish-brown papules and nodules that vary from 1 to 2 mm to several centimeters in diameter.
- Lesions arise singly or in clusters or cobblestone-like crops.
- Mucosal lesions are present in approximately 30% of cases.
- Skin lesions can cause destruction of the cartilage around the ears and nose.
- Multiple small lumps around the nail can occur, known as "coral beads" [2].
- Lesions are usually asymptomatic, but about a third of patients complain of pruritus [2].
Multicentric reticulohistiocytosis can be accompanied by systemic symptoms, including:
- Weightloss
- Fever
- Discomfort
- Myalgia
- Lymphadenopathy [2].
How is multicentric reticulohistiocytosis diagnosed?
Multicentric reticulocytosis is diagnosed from histology of a skin biopsy, showing:
- Multiple multinucleated giant cells
- Histiocytes with eosinophilic cytoplasm and a frosted glass look [1]
- Positive immunohistochemical staining for histiocytes of a monocyte–macrophage origin and an abundance of cytokines, including tumor necrosis alpha factor (TNF-α).
Histiocytes and multinucleated giant cells can also be found in the joints and occasionally in internal organs.
Blood tests are not diagnostic; can include routine hematological research lipid profile, thyroid profile, C-reactive protein (CRP) and rheumatoid factor. Most patients with multicentric reticulohistiocytosis have mild anemia; 30-60% of patients have hyperlipidemia and elevated erythrocytes sedimentation rate (ESR) / C-reactive protein (CRP) [2,3].
A positive tuberculin skin test is found in 12-50% in patients with multicentric reticulohistiocytosis and is more common in tuberculosis endemic [3].
Once the diagnosis of multicentric reticulohistiocytosis has been made, a complete medical history and physical examination with age-appropriate screening tests for malignancy, including a chest radiograph and ultrasound examination of the abdomen / pelvis [1].
What is the treatment for multicentric reticulohistiocytosis?
There is no specific or curative treatment for multicentric reticulohistiocytosis. The following have been reported to be helpful:
- Methotrexate
- Short courses of systemic corticosteroids (prednisolone / oral prednisone)
- Cyclosporine
- Azathioprine
- Cyclophosphamide
- Leflunomide
-
Etanercept [4].
What is the result for multicentric reticulohistiocytosis?
In many patients, multicentric reticulocytosis can enter remission after an average course of 8 years; however, by this time considerable joint destruction may have occurred. Arthritis mutilans can develop in 50% of cases. [2]. Patients are left with deformed and paralyzing joints and a disfigured facial appearance.

